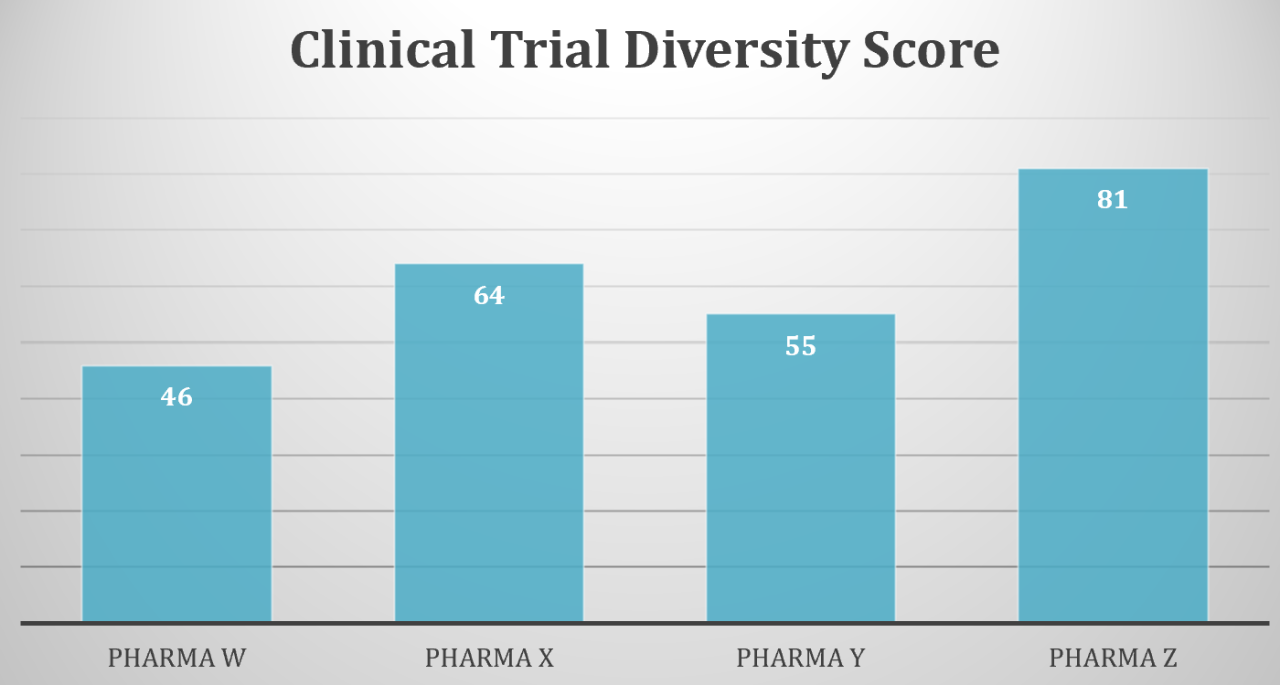
Clinical trials are critical for evaluating the safety and effectiveness of medical devices and pharmaceutical products. The results of trials guide treatment plans, empowering patients and their care teams to make informed decisions about how to manage an acute illness or chronic condition and improve quality of life.
Unfortunately, clinical trial diversity is a longstanding problem in healthcare and life sciences. Communities of color are historically underrepresented in trials. That means researchers – and physicians – don’t know as much about how approved treatments work for these populations as they do for white Americans.
A more inclusive clinical trial process is vital for advancing medical knowledge and helping the healthcare industry rebuild trust with communities of color. Here’s what today’s researchers need to know about addressing diversity in healthcare and the importance of representation in clinical trials.
The Importance of Diversity in Clinical Trials
The National Institute on Minority Health and Health Disparities (NIMHD) notes several benefits of clinical trials. These include determining whether a new intervention is safer or more effective than existing treatments, exploring how to detect diseases earlier, and studying how to improve the quality of life in patients with chronic conditions or acute illnesses. Medical research and advances in healthcare depend on the clinical trial process.
Clinical trials benefit from a diverse population of participants because no two people experience a disease the same way. Differences in biology and genetics may exist among people that can impact how a drug works and how they respond to treatment. (This explains why there seems to be one person in every household who bounces back from the flu faster than everyone else.)
NIMHD pointed out that many factors can influence whether someone develops a disease, as well as how someone responds to a treatment. These include but aren’t limited to age, biological sex, genetic variations, environmental conditions, or additional diseases.
The results of a clinical trial reflect the population that participated in the trial. As Harvard Medical School puts it, “If [trials] only include participants from a narrow demographic group, the results may not accurately represent the broader population.” This may result in treatments that are less effective – or even harmful – to certain segments of the population.
Clinical Trial Diversity: Healthcare and Medical Research Implications
Historically, communities of color have been underrepresented in the clinical trial process. According to the U.S. Food and Drug Administration (FDA), only 11% of participants in new drug trials in 2020 were Hispanic, and only 8% of participants were Black, despite these communities of color making up 19% and 14% of the U.S. population, respectively. In contrast, white Americans make up 60% of the population but 75% of clinical trial participants.
Looking at data from individual trials, representation only gets worse. In a 2022 Lancet study, 10% of clinical trials reported enrollment that was 100% White – while 21% of trials had no Black enrollees and 25% had no Hispanic participants. Similarly, a 2022 Journal of the American Medical Association paper found Americans over the age of 75 are underrepresented in clinical trials relative to their age and disease burden.
This lack of clinical trial diversity poses a problem for many reasons. First, if a clinical trial has no participants from communities of color, then researchers simply don’t know how a treatment will affect those communities. In fact, a 2022 Health Affairs paper concluded that less than 20% of drug trials reported data on specific treatment benefits or side effects for Black patients.
Another issue, a second Lancet paper noted, is that over-representation of white participants is a “stark contrast” to the disease burden in communities of color. Data from the Centers for Disease Control and Prevention (CDC) indicated communities of color have a higher prevalence of obesity and diabetes than white Americans. Additionally, members of communities of color are more likely to receive a late-stage cancer diagnosis, according to the Kaiser Family Foundation. This matters because late-stage cancer generally is more difficult and expensive to treat and has a higher mortality rate than early-stage cancer.
Diversity in Healthcare and the Importance of Representation
In 2022, the FDA took additional steps, releasing a new draft guidance to improve clinical trial diversity that provides recommendations on the approach for developing a Race and Ethnicity Diversity Plan. The agency’s guidance stated researchers “should define enrollment goals for underrepresented racial and ethnic participants as early as practicable in clinical development for a given indication,” with an emphasis on differences in safety or effectiveness associated with race or ethnicity. Critically, this draft guidance represents an important shift: It instructs research sponsors to submit diversity plans to the agency prior to the start of pivotal studies.
That said, the imperative to enhance clinical trial enrollment and diversity is more than a regulatory push. A 2023 New England Journal of Medicine perspective offered three important benefits:
- Earn and rebuild trust. When patients see results from trials with participants with whom they identify, they are more likely to trust the results of the trial – and potentially benefit from a proven treatment.
- Promote fairness. Making it easier for underrepresented populations to participate in clinical trials can “promote fairer distribution of gains in medical knowledge.” This may require steps such as recruiting participants in community-based clinics, limiting the number of required in-person visits, and compensating patients for their time (including travel).
- Advance knowledge. By improving clinical trial diversity, healthcare stakeholders can better understand two things. One is how disease burdens impact communities of color and other populations traditionally underrepresented in trials. The other is how specific treatments work for these populations – and, if they don’t, what questions should drive further research.
Identifying and recruiting more diverse patient populations for trials benefits researchers, patients, and the medical community.
Boost inclusivity in trials faster and for the long term by zeroing in on the populations you lack. Acclinate gives you access to communities of color, facilitates engagement around your trials, and then analyzes the data generated to predict and plan where and when your next effort should happen to create the ongoing representation you need. To learn more, schedule a 1:1 Meeting.