Healthcare has a longstanding history of underrepresentation of communities of color. It often begins with the clinical trial process, where longstanding and well-established mistrust of the industry makes it difficult to recruit Black participants. The impact of the lack of diversity in healthcare and medical research further extends to limited treatment options and poor clinical outcomes for communities of color.
Though efforts to address the issue are long overdue, momentum is building — especially in the field of clinical research, where underrepresentation can critically impact the efficacy of treatment protocols and pharmaceutical development. FDA draft guidance released in 2022 is pushing life science organizations to increase diversity in clinical trials, even before drug therapies and medical devices are close to market. That said, medical research companies cannot underestimate the importance of building trust within communities of color as they rethink how they engage and recruit with populations that have been left on the sidelines.
A History of Exploitation and a Legacy of Mistrust
Examples of unethical treatment of communities of color by medical professionals in the United States aren’t hard to come by.
J. Marion Sims, often considered the father of gynecology, conducted research on enslaved Black women without anesthesia – and arguably without consent – in developing treatments for vesicovaginal fistula in the mid-19th century. Though some argue the women would have otherwise gone untreated, others suggest they endured needless suffering. Sims himself admitted one patient’s “agony was extreme.”
The infamous Tuskegee experiment withheld syphilis treatment from hundreds of Black men for decades in an effort to understand the disease’s long-term progression – even after penicillin was identified as a successful remedy. The experiment ended only after a reporter broke the story in 1972, 40 years after the study began. A subsequent federal investigation concluded, in the words of Tuskegee University, that “scientific research protocol routinely applied to human subjects was either ignored or deeply flawed.”
In 1951, Henrietta Lacks sought treatment for cervical cancer at Johns Hopkins. Without her consent, researchers sampled cells from her cervix. After learning the cells could grow in a lab setting, researchers shared Lacks’ cells. They have since been used to develop treatments for infertility, polio, and COVID-19 – but it wasn’t until August 2023 that Lacks’ family received compensation from the companies that benefited from her cells.
This legacy of unethical behavior and exploitation has caused mistrust. Surveys have shown that Black patients are twice as likely as white patients to believe they will undergo treatment without their consent, as well as one-and-a-half times as likely to believe they would be prescribed experimental medications without their knowledge.
Not surprisingly, this mistrust makes it difficult to recruit individuals from communities of color for clinical trials – which, by their nature, are experimental procedures.
Clinical Trial Representation: Where Do We Stand Now?
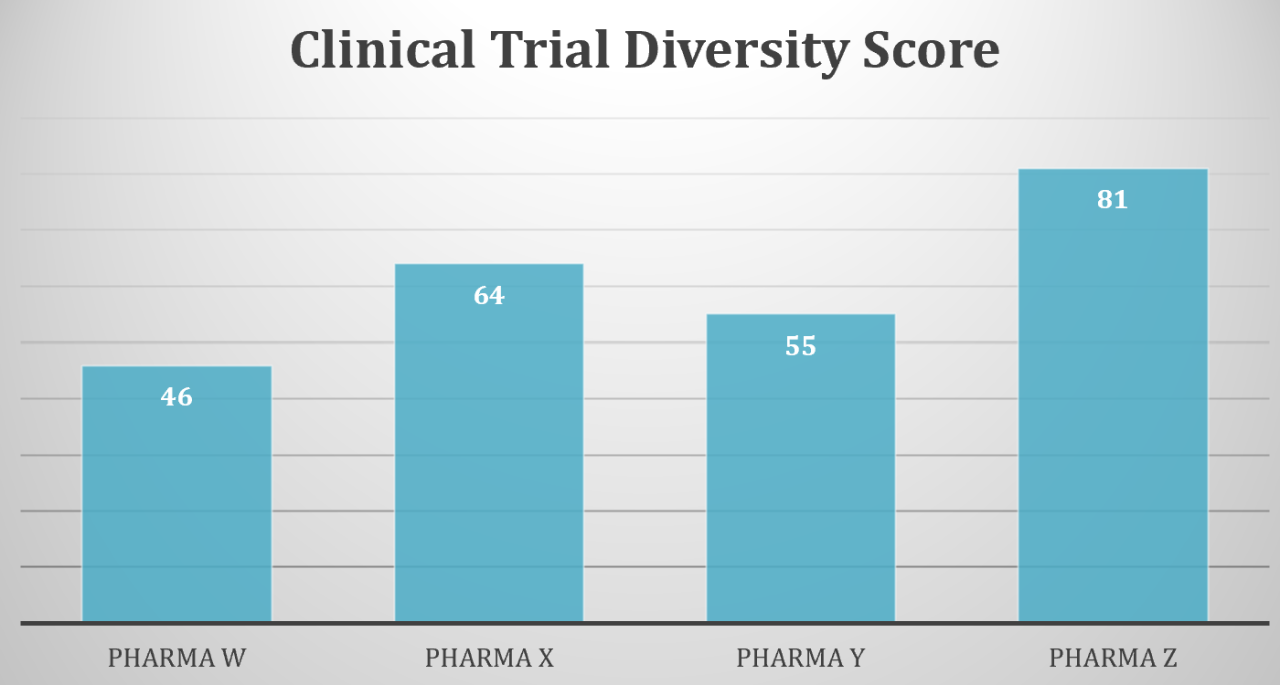
The U.S. Food and Drug Administration (FDA) reports that in 2020, only 11% of participants in new drug trials were Hispanic, and only 8% of participants were Black. These communities of color comprise 19% and 14% of the U.S. population, respectively. Meanwhile, a 2022 Lancet literature review found 25% of clinical trials had no Hispanic enrollees, and 21% had no Black enrollees.
Underrepresentation in clinical trials has a significant downstream impact on health disparities, as practitioners have limited data about which treatment options work best in non-white patients. In fact, the Centers for Disease Control and Prevention (CDC) reported patients from communities of color have a higher prevalence of obesity and diabetes than white Americans.
There’s an economic cost as well. The diagnosis of a chronic condition makes it difficult for someone to work, decreases their life expectancy, and increases healthcare spending. Research from the University of Southern California suggested that if increasing clinical trial diversity led to just a 1% improvement in disparities, economic gains on the order of $40 billion for diabetes and $60 billion could be realized. That’s a substantial dent in the nation’s ever-rising healthcare spending – and a significant impact on the quality of life in communities of color feeling the effects of unethical medicine and systemic racism.
The Health Equity and Accountability Act: Overdue Efforts Gain Momentum
Since 2003, members of the Congressional Tri-Caucus have periodically introduced the Health Equity and Accountability Act. Most recently re-released in 2022, the bill strives to evaluate health disparities, strengthen health data collection and healthcare research, improve diversity in healthcare’s workforce, address systemic barriers to accessing care, and assess environmental factors that influence health. To date, more than 300 health equity organizations have helped shape the bill.
No action was taken on the bill, and its history of introduction and referral to committee means it may be some time before the Health Equity and Accountability Act officially becomes law. However, other recent activity on Capitol Hill shows elected officials and federal agencies are beginning to get serious about how to improve diversity, equity, and inclusion in healthcare and life sciences.
The aforementioned FDA draft guidance on improving diversity in clinical trial enrollment is an important step forward. Additionally, the Food and Drug Omnibus Reform Act of 2022 (FDORA) specifically requires a “diversity action plan” for certain late-stage trials for drugs and devices. FDORA also pushes the FDA to issue guidance for conducting decentralized clinical trials, which is a valuable practice for increasing enrollment and ongoing participation among communities of color and other underrepresented populations.
How to Improve Diversity, Equity, and Inclusion in Clinical Trials
There are clear regulatory, business, and ethical reasons for the industry to improve representation in clinical trials. However, it’s not enough to identify communities of color for possible enrollment. It’s imperative to connect with these communities – to build trust where it hasn’t existed before, provide resources respectful of and tailored to communities of color, and advocate for measurable and meaningful change with active engagement. Only then will diversity in healthcare and life sciences become effective for your business — and start to become standard practice.
Boost inclusivity in trials faster and for the long term by zeroing in on the populations you lack. Acclinate gives you access and authentic connection to communities of color through NOWINCLUDED, a trusted health education and engagement source created by and for the Black/African American community. We then facilitate engagement around your trials, analyzing the data generated to predict and plan where and when your next effort should happen to create the ongoing representation you need. To learn more, schedule a 1:1 meeting.